Photo by sayan Nath on Unsplash
Hey there everyone –
People are socialized to bring therapists their pain and to expect relief. To see a mental health practitioner as a kind of “brain doctor”: a person who has been trained to diagnose, to offer a treatment, to solve a person’s problem because they know what treatment works for a certain diagnosis and what treatment won’t help.
I’m talking about the mainstream model here, the one that’s reinforced by institutions that offer the continuing education courses mental health practitioners have to take to keep their license in good standing; the ones that create the licensure exam questions; that see evidence-based practices as the gold standard of care; that require a treatment plan with measurable outcomes against which to track a patient’s progress.
This model of care was institutionalized in 1980, with the publication of the Diagnostic and Statistical Manual III. There was a big nerdy fight in the American Psychiatric Association and across the field in the years leading up to its publication, and eventually psychoanalysis, the former framework through which most “neuroses” and “psychoses” were understood, was chucked, and the medical model won.
What appears today to be the normal and usual way of thinking about mental health, that is, is a rather recent creation. Or, more specifically, is a re-emergence of a way of looking at mental illness that has its roots in the nineteenth century. Part of the reason the field was in crisis in the late 70s was due to some inconvenient questions posed by the anti-psychiatry movement, which had its roots in the social justice movements of the late ‘60s. The people active in this movement started to question the ways schools, hospitals, prisons and the Law worked together to “manage” people, often through systems that used therapeutic methods and languages to justify their approach.
The anti-psychiatry movement put the field on the defensive, and one way it decided to respond to the challenge was to rigorously test its own methods. To ask if it had the standing to consider itself a science, like medicine. And if it failed that test, to see what it would take to make mental health a scientifically rigorous discipline, rooted in reason and objectivity and a universal standard of care.
This battle, which seemed to have ended in 1980, pushed approaches that didn’t fit the medical model to the margins. It succeeded in reinforcing the standard of care, in making sure large research grants went mostly to quantitative studies that track one or two variables of measurement, rather than qualitative studies, which ask questions that generate narrative rather than statistical results. (I’m oversimplifying here, of course, but this is a trend.)
I don’t think it’s a coincidence that the turn back to the medical model in 1980 coincided with the victory of Reagan, the slashing of social services, the re-containing of the social justice movements and the dominant culture’s celebration of bootstrap individualism as the quality that made America a great and distinctive nation. So for today, I thought I’d introduce some of the questions that were raised by the anti-psychiatry movement, because I think they’re coming back. As questions about the mental health impacts of climate, war, police brutality, sexual and gender-based violence are part of everyday conversation, and are being explicitly politicized, it is getting harder, again, to see mental health as something that individuals, alone, can manage and solve.
So here’s some questions to ask yourself and your friends about mental health:
Is therapy a method of helping people “adjust” to a system that is in itself unjust, violent, and cruel? A way of teaching people to tolerate their own pain and that of others?
Does the focus on diagnosis and treatment teach the patient or client to view themselves as both the source of distress and at the same time the one who has the power to get better?
What is the ultimate source of mental distress? Is it a malfunction of the brain’s neurochemistry? Is it a hereditary or genetic disorder? Is it a thinking pattern that has taken on an energy of its own, that requires interruption?
How does a therapist know what “mental health” looks like? How do they learn what “disorder” looks like? What behaviors indicate that someone is “healthy” and by extension “unhealthy”?
If therapy is a place for conversations about issues that aren’t about the individual’s thoughts and behaviors; if therapy is a place where broad social issues are also included in conversation, what does “treatment” look like, in this context?
Just to be clear, I’m not saying the medical model isn’t a good way of thinking about care, or mental illness, or distress. Rather, I’m seeing this moment in time as one in which the questions that were pushed out of the frame in the 1980s are coming back, and putting these questions in relation to the current mainstream way of thinking expands our understanding of what we assume “mental health” looks like, how it is attained, and what is necessary to create it, for all of us.
Stay safe out there this week–
xo
Rebecca
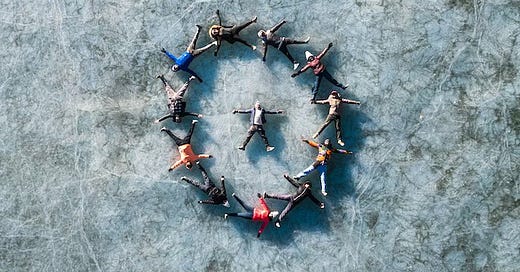

I see individual therapy as isolated from our other relationships. I see us try to bridge this gap by starting sentences with “my therapist told me” but the statements that follow can often land flatly. Result is a decrease in connection with the people in the present moment rather than an increase.
Really interesting history. And great questions.